Diagnosis and treatment of penetrating orbital cranial foreign body injuries
Main Article Content
Abstract
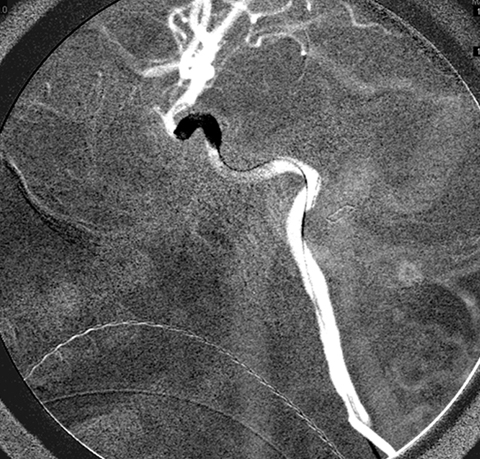
Although periorbital trauma may appear trivial externally, ophthalmic findings of decreased vision, decreased motility, or of any neurological derangement should raise suspicion for more serious injury. In such cases, particularly in children (who may resist revealing the details of the injury), the possibility of a retained foreign body must also be considered. Initial neuroimaging in the form of CT should be carefully reviewed, and concern for a retained foreign body should also be communicated directly to the radiologist, preferably a neuroradiologist. The treating clinician should directly review all imaging studies and not simply rely on written reports. Wooden foreign bodies typically appear as aerated structures and widening of window width and level on CT scans can be helpful in revealing a linear course and overall geometric structure that is highly suspicious for a clinically occult wooden foreign body. If there is any concern for intracranial injury, neurosurgery should be consulted. Special studies, such as CT angiography or formal digital subtraction cerebral angiography, may be warranted to further assess vascular integrity. The foreign body should be extracted as safely as possible, either via anterior orbitotomy or craniotomy taking into account adjunctive measures that may be required to prevent or emergently control potentially life threatening hemorrhage.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Shoeb Ahmad S, Ghani SA, Peng KS, Sellamuthu P. 5-year-old girl with left upper eyelid swelling. Digital J Ophthalmol 2012;18. December 31, 2012. DOI: https://doi.org/10.5693/djo.03.2012.05.001
Shelsta HN, Bilyk JR, Rubin PAD, Penne RB, Carrasco JR. Wooden Intraorbital foreign body injuries: clinical characteristics and outcomes of 23 patients. Ophthal Plast Reconstr Surg 2010;26:238-44. DOI: https://doi.org/10.1097/IOP.0b013e3181bd7509
Carothers A. Orbitofacial wounds and cerebral artery injuries caused by umbrella tips. JAMA 1978;239:1151-2. DOI: https://doi.org/10.1001/jama.239.12.1151
Schreckinger M, Orringer D, Thompson BG, La Marca F, Sagher O. Transorbital penetrating injury: case series, review of the literature, and proposed management algorithm. J. Neurosurg 2011;114:53-61. DOI: https://doi.org/10.3171/2010.8.JNS10301
Dunn IF, Kim DH, Rubin PA, Blinder R, Gates J, Golby AJ. Orbitocranial wooden foreign body: a pre-, intra-, and postoperative chronicle: case report. Neurosurgery 2009;65:E383-4; discussion E384. DOI: https://doi.org/10.1227/01.NEU.0000347474.69080.A1
Cunningham EJ, Albani B, Masaryk TJ, Rasmussen PA. Temporary balloon occlusion of the cavernous carotid artery for removal of an orbital and intracranial foreign body: case report. Neurosurgery 2004;55:1225. DOI: https://doi.org/10.1227/01.NEU.0000140991.82075.01
Fezza J, Wesley R. The importance of CT scans in planning the removal of orbital-frontal lobe foreign bodies. Ophthal Plast Reconstr Surg 1999;15:366-8. DOI: https://doi.org/10.1097/00002341-199909000-00012
Hern JD, Coley SC, Hollis LJ, Jayaraj SM. Delayed massive epistaxis due to traumatic intracavernous carotid artery pseudoaneurysm. J Laryngol Otol 1998;112:396-8. DOI: https://doi.org/10.1017/S0022215100140575