Paracentral acute middle maculopathy
Main Article Content
Abstract
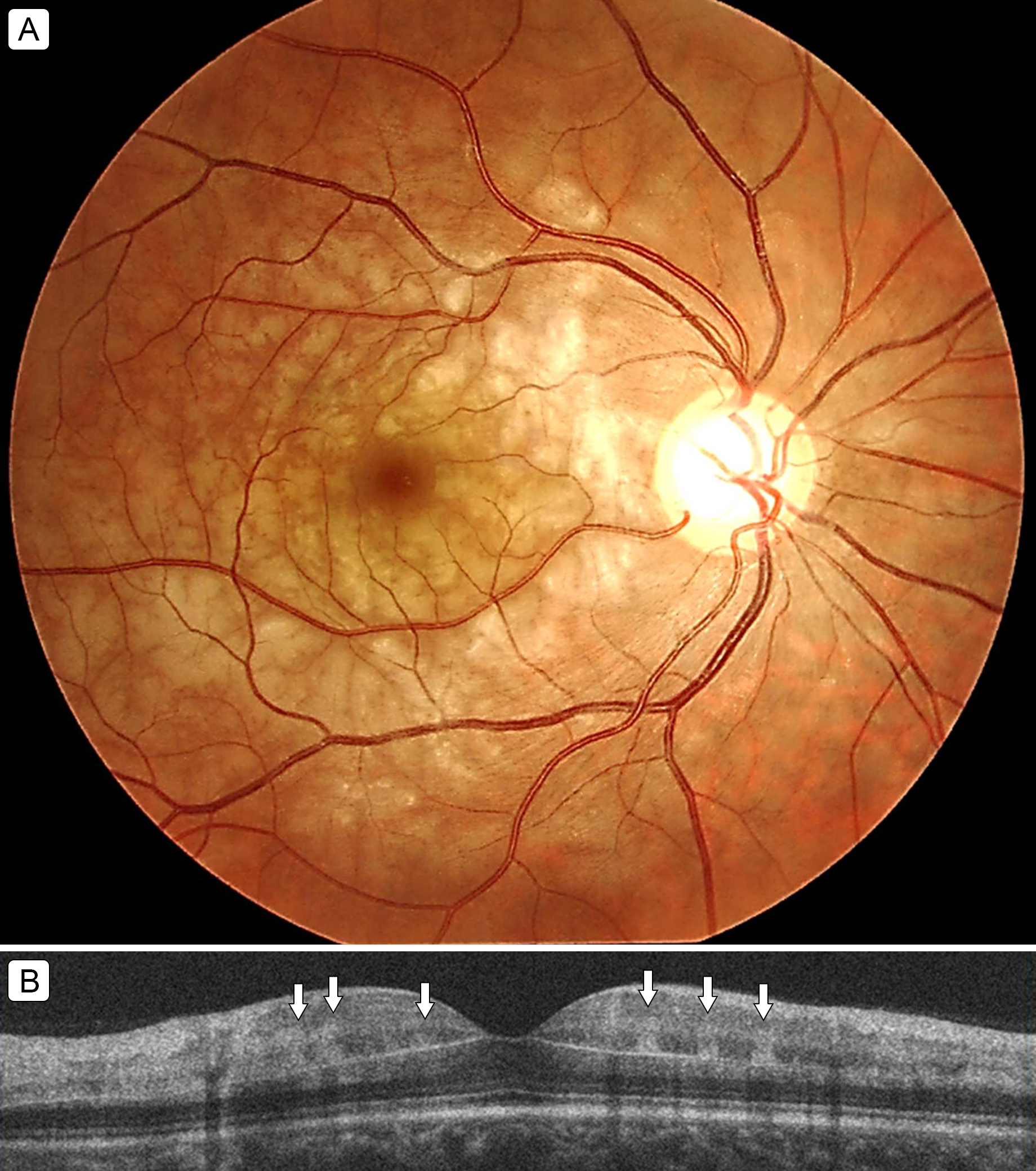
A 30-year-old man presented at Inoda Eye Clinic with transient blindness in the right eye. At the time of presentation, he had been experiencing gradual improvement of symptoms. On examination, visual acuity was 0.6 in the affected eye, with a relative afferent pupillary defect. Ophthalmoscopic examination revealed fernlike retinal edema in the right eye (A); however, no cherry-red spot was detected. Optical coherence tomography showed hyperreflective bandlike lesions involving the middle layers of the retina at the level of the inner nuclear layer (B, arrows). Based on these findings, the patient was diagnosed with paracentral acute middle maculopathy (PAMM) due to incomplete central retinal artery occlusion. PAMM is a clinical sign of ischemia of the deep retinal vascular layers. During the 2-week follow-up, without treatment, retinal edema gradually decreased, and visual acuity improved to 1.2. After recovery from this event, the patient experienced no additional periods of transient blindness during 3 months of follow-up.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.