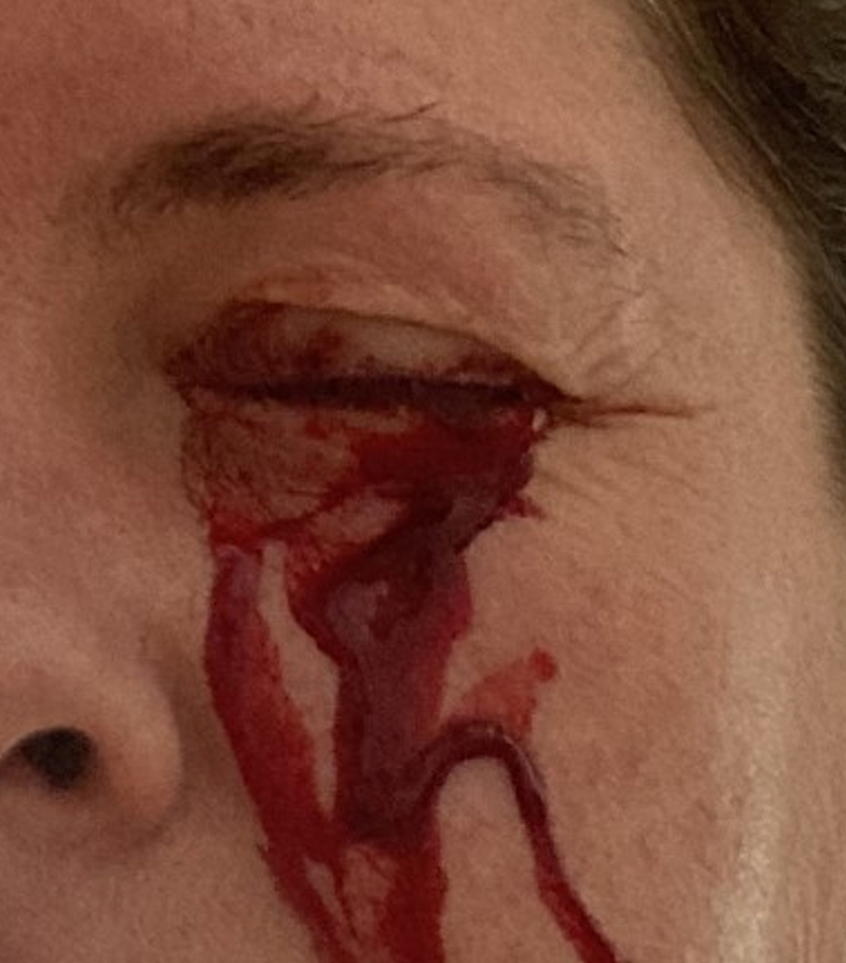
A 43-year-old woman with nontraumatic profuse ocular hemorrhage
Main Article Content
Abstract
A 43-year-old white woman presented emergently with sudden-onset, extensive bleeding from the left eye of one day’s duration, without pain, visual disturbance, trauma, or systemic symptoms. She had no significant ophthalmic, medical, surgical, or social history and did not wear contact lenses. Initial emergency department assessment revealed no eyelid laceration, penetrating injury, or identifiable source of bleeding. On same-day ophthalmic examination, her best-corrected visual acuity was 6/6 in both eyes, and pupillary responses were normal, without a relative afferent pupillary defect. Examination of the right eye was unremarkable. The left eye showed mild conjunctival hyperemia, a clear cornea, a deep and quiet anterior chamber, and a localized vascularized lesion on the superior lateral palpebral conjunctiva. Fundus examination was normal bilaterally. Initial investigations, including blood tests and orbital computed tomography, were normal. The lesion was suspected to be a pyogenic granuloma. Topical steroid–antibiotic treatment was unsuccessful. Excisional biopsy confirmed that the lesion was a benign vascular lesion composed of lobulated capillaries with inflammatory infiltrate and no malignant features, explaining the rare presentation of hemolacria.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Tripathy K, Salini B. Hemolacria. August 25, 2023. In: StatPearls. Treasure Island, FL: StatPearls Publishing; 2025-.
Chon BH, Zhang R, Bardenstein DS, Coffey M, Collins AC. Bloody epiphora (hemolacria) years after repair of orbital floor fracture. Ophthalmic Plast Reconstr Surg 2017;33:e118-e120.
Ferry AP, Pyogenic granulomas of the eye and ocular adnexa: a study of 100 cases. Trans Am Ophthalmol Soc 1989;87:327-43; discussion 343-7.
Tan IJ, Turner AQ. Pyogenic granuloma of the conjunctiva. N Engl J Med 2017;376:1667.
Honavar SG, Manjandavida FP. Tumors of the ocular surface: a review. Indian J Ophthalmol 2015;63:187-203.
Patten J, Hynduik R. Granuloma pyogenicum of the conjunctiva. Ann Ophthalmol 1975;7:1588-90.
Sehu KW, Lee WR. Ophthalmic Pathology: an Illustrated Guide for Clinicians. Hoboken, NJ, USA. : John Wiley & Sons; 2012.
Espinoza GM, Lueder GT. Conjunctival pyogenic granulomas after strabismus surgery. Ophthalmology 2005;112:1283-6.
Wu D, Qian T, Nakao T, et al. Medically uncontrolled conjunctival pyogenic granulomas: correlation between clinical characteristics and histological findings. Oncotarget 2016;8:2020-24.
Oke I, Alkharashi M, Petersen RA, Ashenberg A, Shah AS. Treatment of ocular pyogenic granuloma with topical timolol. JAMA Ophthalmol 2017;135:383-5.