Complications following incisional glaucoma surgery, minimally invasive glaucoma surgery, and cycloablative procedures: a 13-year retrospective review
Main Article Content
Abstract
Purpose
To evaluate the incidence, clinical course, and treatment outcomes of glaucoma surgery–related infections at a tertiary academic center over a 13-year time period.
Methods
Patients presenting at Duke Eye Center between January 1, 2010, and November 11, 2023, who underwent glaucoma surgery, including trabeculectomy, glaucoma drainage device (GDD) placement, GDD revision surgery, trabeculectomy bleb revision surgery, minimally invasive glaucoma surgery (MIGS), Xen gel stent implantation, and cycloablative procedures, were identified using an electronic medical record clinical database search. Diagnosis of blebitis, bleb-associated endophthalmitis, and tube malposition or tube exposure were determined using International Classification of Disease (9th and 10th editions) codes.
Results
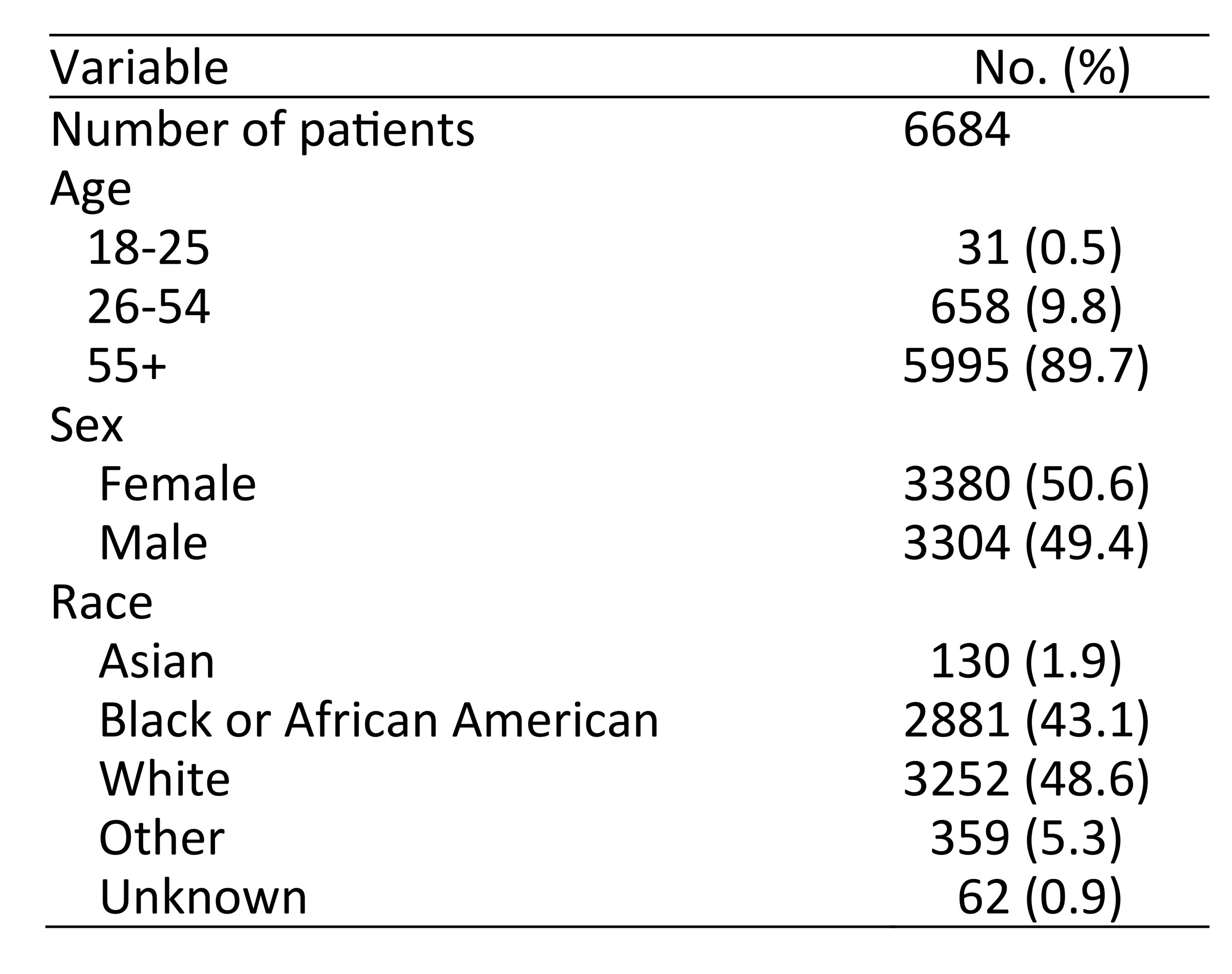
A total of 12,115 glaucoma surgeries (in 6,684 patients) were identified during the study period. GDD implantation comprised the majority of glaucoma surgeries (33%), followed by trabeculectomy (with and without Ex-PRESS mini glaucoma shunt) (25.7%), GDD revision (8.9%), trabeculectomy bleb revision (8.6%), and transscleral cyclophotocoagulation (5.9%). There were 488 MIGS with and without phacoemulsification (4%) and 76 Xen gel stent surgeries (0.6%). Endophthalmitis was diagnosed in 18 eyes (0.96%) that underwent trabeculectomy, 11 eyes that underwent GDD implantation (0.20%), and 1 eye that underwent Xen stent implantation. Blebitis was diagnosed in 7 eyes: 5 were related to trabeculectomy (0.27%), and 2 were related to GDD placement (0.05%). The incidence of GDD malposition or erosion was 10.2%. No cases of endophthalmitis were diagnosed in patients with MIGS.
Conclusions
In our study cohort, infectious complications associated with trabeculectomy and GDD implant surgery were low; there were no cases of endophthalmitis associated with MIGS. The rate of GDD complications due to tube malposition or erosion was 10.2%.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Zheng CX, Moster MR, Khan MA, et al. Infectious endophthalmitis after glaucoma drainage implant surgery: clinical features, microbial spectrum, and outcomes. Retina 2017;37:1160-7. DOI: https://doi.org/10.1097/IAE.0000000000001329
Reynolds AC, Skuta GL, Monlux R, Johnson J. Management of blebitis by members of the American Glaucoma Society: a survey. J Glaucoma 2001;10:340-7. DOI: https://doi.org/10.1097/00061198-200108000-00015
Medina CA, Butler MR, Deobhakta AA, et al. Endophthalmitis associated with glaucoma drainage implants. Ophthalmic Surg Lasers Imaging Retina 2016;47:563-9. DOI: https://doi.org/10.3928/23258160-20160601-08
Gedde SJ, Scott IU, Tabandeh H, et al. Late endophthalmitis associated with glaucoma drainage implants. Ophthalmology 2001;108:1323-7. DOI: https://doi.org/10.1016/S0161-6420(01)00598-X
Al-Torbak AA. Endophthalmitis associated with the Ahmed glaucoma valve implant. Br J Ophthalmol 2005;89:454-8. DOI: https://doi.org/10.1136/bjo.2004.049015
Greenfield DS. Endophthalmitis after filtering surgery with mitomycin. Arch Ophthalmol 1996;114:943. DOI: https://doi.org/10.1001/archopht.1996.01100140151007
DeBry PW. Incidence of late-onset bleb-related complications following trabeculectomy with mitomycin. Arch Ophthalmol 2002;120:297. DOI: https://doi.org/10.1001/archopht.120.3.297
Higginbotham EJ, Stevens RK, Musch DC, Karp KO, Lichter PR, Bergstrom TJ, et al. Bleb-related endophthalmitis after trabeculectomy with mitomycin C. Ophthalmology 1996;103:650-6. DOI: https://doi.org/10.1016/S0161-6420(96)30639-8
Vaziri K, Kishor K, Moshfeghi D, et al. Incidence of bleb-associated endophthalmitis in the United States. Clin Ophthalmol 2015;9:317-22. DOI: https://doi.org/10.2147/OPTH.S75286
Yamamoto T, Sawada A, Mayama C, et al. The 5-year incidence of bleb-related infection and its risk factors after filtering surgeries with adjunctive mitomycin C. Ophthalmology 2014;121:1001-6. DOI: https://doi.org/10.1016/j.ophtha.2013.11.025
Katz LJ, Cantor LB, Spaeth GL. Complications of surgery in glaucoma: Early and late bacterial endophthalmitis following glaucoma filtering surgery. Ophthalmology 1985;92:959-63. DOI: https://doi.org/10.1016/S0161-6420(85)33948-9
Mac I, Soltau JB. Glaucoma-filtering bleb infections. Curr Opin Ophthalmol 2003;14:91-4. DOI: https://doi.org/10.1097/00055735-200304000-00007
Nguyen QH. Complications of Baerveldt glaucoma drainage implants. Arch Ophthalmol 1998;116:571. DOI: https://doi.org/10.1001/archopht.116.5.571
Simonett JM, Choi RY, Flaxel CJ. Filtering-associated endophthalmitis after trabeculectomy or tube-shunt implant. Ophthalmol Retina 2021;5:279-84. DOI: https://doi.org/10.1016/j.oret.2020.07.013
Levinson JD, Giangiacomo AL, Beck AD, et al. Glaucoma drainage devices: risk of exposure and infection. Am J Ophthalmol 2015;160:516-21.e2. DOI: https://doi.org/10.1016/j.ajo.2015.05.025
Francis BA, Singh K, Lin SC, et al. Novel glaucoma procedures. Ophthalmology 2011;118:1466–80. DOI: https://doi.org/10.1016/j.ophtha.2011.03.028
Mathew DJ, Buys YM. Minimally invasive glaucoma surgery: a critical appraisal of the literature. Annu Rev Vis Sci 2020;6:47-89. DOI: https://doi.org/10.1146/annurev-vision-121219-081737
Ishida K. Update on results and complications of cyclophotocoagulation: Curr Opin Ophthalmol 2013;24:102-10. DOI: https://doi.org/10.1097/ICU.0b013e32835d9335
Amoozgar B, Phan EN, Lin SC, Han Y. Update on ciliary body laser procedures. Curr Opin Ophthalmol 2017;28:181-6. DOI: https://doi.org/10.1097/ICU.0000000000000351
Lim R. The surgical management of glaucoma: a review. Clin Experiment Ophthalmol 2022;50:213-31. DOI: https://doi.org/10.1111/ceo.14028
Gedde SJ, Herndon LW, Brandt JD, Budenz DL, Feuer WJ, Schiffman JC. Postoperative complications in the tube versus trabeculectomy (TVT) study during five years of follow-up. Am J Ophthalmol 2012;153:804-14.e1. DOI: https://doi.org/10.1016/j.ajo.2011.10.024
Wallin Ö, Al‐ahramy AM, Lundström M, Montan P. Endophthalmitis and severe blebitis following trabeculectomy: epidemiology and risk factors; a single‐centre retrospective study. Acta Ophthalmol (Copenh) 2014;92:426-31. DOI: https://doi.org/10.1111/aos.12257
Trubnik V, Zangalli C, Moster MR, et al. Evaluation of risk factors for glaucoma drainage device–related erosions: a retrospective case-control study. J Glaucoma 2015;24:498-502. DOI: https://doi.org/10.1097/IJG.0000000000000034
Al-Beishri AS, Malik R, Freidi A, Ahmad S. Risk factors for glaucoma drainage device exposure in a Middle-Eastern population. J Glaucoma 2019;28:529-34. DOI: https://doi.org/10.1097/IJG.0000000000001220
Zhou D, Zhou X, Mas-Ramirez A, et al. Factors associated with conjunctival erosions after Ahmed glaucoma valve implantation. J Ophthalmic Vis Res 2018;13:411. DOI: https://doi.org/10.4103/jovr.jovr_219_17
Muir KW, Lim A, Stinnett S, Kuo A, Tseng H, Walsh MM. Risk factors for exposure of glaucoma drainage devices: a retrospective observational study. BMJ Open 2014;4:e004560. DOI: https://doi.org/10.1136/bmjopen-2013-004560
Budenz DL, Feuer WJ, Barton K, et al. Postoperative complications in the Ahmed Baerveldt comparison study during five years of follow-up. Am J Ophthalmol 2016;163:75-82.e3. DOI: https://doi.org/10.1016/j.ajo.2015.11.023
Christakis PG, Kalenak JW, Tsai JC, et al. The Ahmed versus Baerveldt study. Ophthalmology 2016;123:2093-102. DOI: https://doi.org/10.1016/j.ophtha.2016.06.035
Cardakli N, Friedman DS, Boland MV. Unplanned return to the operating room after tube shunt surgery. Am J Ophthalmol 2021;229:242-52. DOI: https://doi.org/10.1016/j.ajo.2021.05.010
Vinod K, Gedde SJ. Safety profile of minimally invasive glaucoma surgery. Curr Opin Ophthalmol 2021;32:160-8. DOI: https://doi.org/10.1097/ICU.0000000000000731
Chaves AC, Grosinger AJ, Ten Hulzen RD, Stewart MW, Dorairaj SK. Endophthalmitis following combined cataract extraction and placement of an iStent trabecular bypass device. Am J Ophthalmol Case Rep 2020;20:100830. DOI: https://doi.org/10.1016/j.ajoc.2020.100830
Starr MR, Huang D, Israilevich RN, et al. Endophthalmitis after minimally invasive glaucoma surgery. Ophthalmology 2021;128:1777-9. DOI: https://doi.org/10.1016/j.ophtha.2021.06.004
Sabharwal J, Dai X, Dun C, et al. Early endophthalmitis incidence and risk factors after glaucoma surgery in the Medicare population from 2016 to 2019. Ophthalmology 2023;131:S0161642023006656. DOI: https://doi.org/10.1016/j.ophtha.2023.09.008
Traverso CE, Carassa RG, Fea AM, et al. Effectiveness and safety of Xen gel stent in glaucoma surgery: a systematic review of the literature. J Clin Med 2023;12:5339. DOI: https://doi.org/10.3390/jcm12165339
Olgun A, Imamoğlu S, Karapapak M, Düzgün E, Kaçar H. Endophthalmitis after XEN gel stent implantation: 2 cases. J Glaucoma 2018;27:e191-4. DOI: https://doi.org/10.1097/IJG.0000000000001076
Lim R, Lim KS. XEN implant-related endophthalmitis. Ophthalmology 2018;125:209. DOI: https://doi.org/10.1016/j.ophtha.2017.10.019
Lin BR, Al-Khersan H, Bitrian E, Flynn HW. Endophthalmitis associated with XEN stent implantation. Am J Ophthalmol 2023;253:37–43. DOI: https://doi.org/10.1016/j.ajo.2023.04.006
Sng CC, Wang J, Hau S, Htoon HM, Barton K. XEN‐45 collagen implant for the treatment of uveitic glaucoma. Clin Experiment Ophthalmol 2018;46:339-45. DOI: https://doi.org/10.1111/ceo.13087
Kono Y, Kasahara M, Hirasawa K, et al. Long-term clinical results of trabectome surgery in patients with open-angle glaucoma. Graefes Arch Clin Exp Ophthalmol 2020;258:2467-76. DOI: https://doi.org/10.1007/s00417-020-04897-0
Khan A, Riaz KM, Rangu N, Shah VA, Hussain ZS, Khaimi MA. Incidence and clinical characteristics of postoperative endophthalmitis after ab-interno canaloplasty. Clin Ophthalmol 2022;16:3875-82. DOI: https://doi.org/10.2147/OPTH.S392322
Nirappel A, Klug E, Neeson C, et al. Transscleral vs endoscopic cyclophotocoagulation: safety and efficacy when combined with phacoemulsification. BMC Ophthalmol 2023;23:129. DOI: https://doi.org/10.1186/s12886-023-02877-6