Association of stage of diabetic retinopathy on intraocular pressure
Main Article Content
Abstract
Purpose
To determine whether stage of diabetic retinopathy (DR) is associated with increased intraocular pressure (IOP).
Methods
The medical records of patients seen in the outpatient ophthalmology clinic at Sidney & Lois Eskenazi Community Hospital in Indianapolis, Indiana, from January 2022 to August 2023 were reviewed retrospectively. The highest IOP of those presenting without type 2 diabetes mellitus (T2DM), T2DM without DR, and varying severity of DR was recorded. Main outcome measures included median and average IOPs recorded from patients who presented without diabetes, diabetes without retinopathy, and mild, moderate, severe nonproliferative and proliferative diabetic retinopathy. Comparisons between groups generated P values, with ≤0.05 indicating statistical significance.
Results
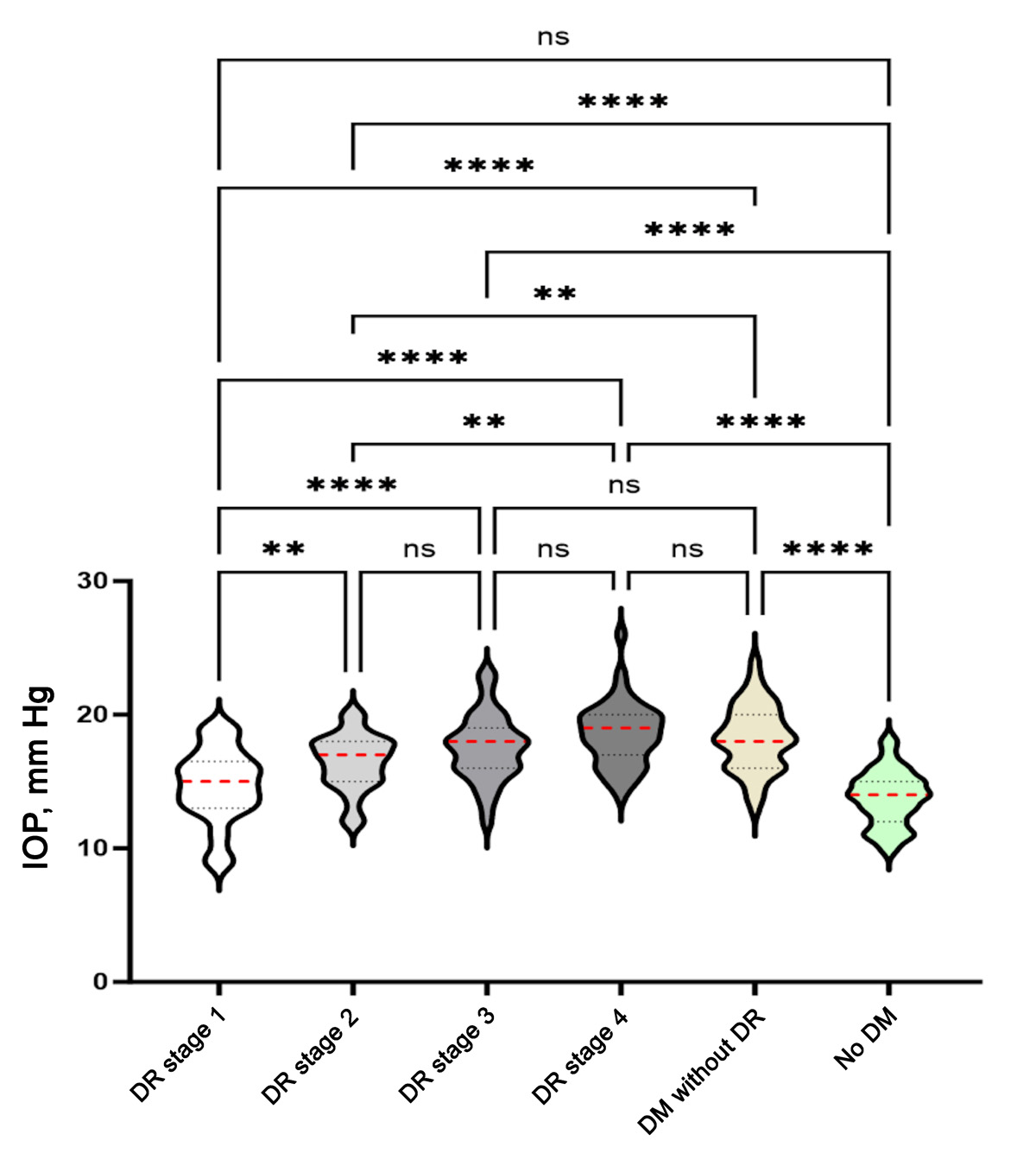
A total of 389 patients (759 eyes) were included. Mean patient age was 58. Male patients accounted for 286 eyes (37.7%); Hispanic patients, for 270 eyes (35.6%); patients identifying as black, for 261 eyes (34.4%); white patients, for 195 eyes (25.7%); and Asian patients, for 33 eyes (4.3%). Overall, analysis showed IOP increased between eyes without T2DM compared with mild nonproliferative DR (P = 0.0373), mild DR compared to moderate nonproliferative DR (P = 0.0117), and moderate DR compared with severe nonproliferative DR (P = 0.0001). The IOP observed between severe nonproliferative DR to proliferative DR (P = 0.5351) was not statistically significant.
Conclusions
In our study cohort, there was a positive correlation between elevated IOP and more advanced stage of DR, indicating that patients with diabetes but no findings of DR on retinal examination seem to be at greater risk of elevated IOP than those with mild-to-moderate DR. These results suggest that IOP in patients with T2DM, with or without DR, should be closely monitored over time to prevent future IOP-related complications.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Allison K, Patel D, Alabi O. Epidemiology of glaucoma: the past, present, and predictions for the future. Cureus 2020;12:e11686.
Zhou M, Wang W, Huang W, Zhang X. Diabetes mellitus as a risk factor for open-angle glaucoma: a systematic review and meta-analysis. PLoS One 2014;9:e102972.
Weinreb RN, Aung T, Medeiros FA. The pathophysiology and treatment of glaucoma: a review. JAMA 2014;311:1901-11.
Goel M, Picciani RG, Lee RK, Bhattacharya SK. Aqueous humor dynamics: a review. Open Ophthalmol J 2010;4:52-9.
Cohen LP, Pasquale LR. Clinical characteristics and current treatment of glaucoma. Cold Spring Harb Perspect Med 2014;4:a017236.
Sun H, Saeedi P, Karuranga S, et al. IDF Diabetes Atlas: Global, regional, and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract 2022;183:109119. [Published correction appears in Diabetes Res Clin Pract. 2023 Oct;204:110945
Stumvoll M, Goldstein BJ, van Haeften TW. Type 2 diabetes: pathogenesis and treatment. Lancet 2008;371:2153-6.
Ko F, Boland MV, Gupta P, et al. Diabetes, triglyceride levels, and other risk factors for glaucoma in the National Health and Nutrition Examination Survey 2005-2008. Invest Ophthalmol Vis Sci 2016;57:2152-7.
Mitchell P, Smith W, Chey T, Healey PR. Open-angle glaucoma and diabetes: the Blue Mountains Eye Study, Australia. Ophthalmology 1997;104:712-8.
Klein BE, Klein R, Jensen SC. Open-angle glaucoma and older-onset diabetes: the Beaver Dam Eye Study. Ophthalmology 1994;101:1173-7.
Heng LZ, Comyn O, Peto T, Tadros C, Ng E, Sivaprasad S, Hykin PG. Diabetic retinopathy: pathogenesis, clinical grading, management and future developments. Diabet Med 2013;30:640-50.
Engerman RL. Pathogenesis of diabetic retinopathy. Diabetes 1989;38:1203-6.
Kollias AN, Ulbig MW. Diabetic retinopathy: early diagnosis and effective treatment. Dtsch Arztebl Int 2010;107:75.
Hymowitz MB, Chang D, Feinberg EB, Roy S. Increased intraocular pressure and hyperglycemic level in diabetic patients. PLoS One 2016;11:e0151833.
Pimentel LG, Gracitelli CP, da Silva LS, Souza AK, Prata TS. Association between glucose levels and intraocular pressure: pre-and postprandial analysis in diabetic and nondiabetic patients. J Ophthalmol 2015;2015:832058.
Yang Y, Zhang X, Chen Z, et al. Intraocular pressure and diurnal fluctuation of open-angle glaucoma and ocular hypertension: a baseline report from the LiGHT China trial cohort. Br J Ophthalmol 2023;107:823-7.
Matlach J, Bender S, König J, Binder H, Pfeiffer N, Hoffmann EM. Investigation of intraocular pressure fluctuation as a risk factor of glaucoma progression. Clin Ophthalmol 2019;13:9-16.
Song BJ, Aiello LP, Pasquale LR. Presence and risk factors for glaucoma in patients with diabetes. Curr Diab Rep 2016;16:1-3.
Zhao D, Cho J, Kim MH, Friedman DS, Guallar E. Diabetes, fasting glucose, and the risk of glaucoma: a meta-analysis. Ophthalmology 2016;122:72-8.
Dielemans I, de Jong PT, Stolk R, Vingerling JR, Grobbee DE, Hofman A. Primary open-angle glaucoma, intraocular pressure, and diabetes mellitus in the general elderly population. The Rotterdam Study. Ophthalmology 1996;103:1271-5.
Tielsch JM, Katz J, Quigley HA, Javitt JC, Sommer A. Diabetes, intraocular pressure, and primary open-angle glaucoma in the Baltimore Eye Survey. Ophthalmology 1995;102:48-53.
Sato T, Roy S. Effect of high glucose on fibronectin expression and cell proliferation in trabecular meshwork cells. Invest Ophthalmol Vis Sci 2002;43:170-5.
Park CH, Kim JW. Effect of advanced glycation end products on oxidative stress and senescence of trabecular meshwork cells. Korean J Ophthalmol 2012;26:123-31.
Geraldes P, King GL. Activation of protein kinase C isoforms and its impact on diabetic complications. Circ Res 2010;106:1319-31.
Vranka JA, Kelley MJ, Acott TS, Keller KE. Extracellular matrix in the trabecular meshwork: intraocular pressure regulation and dysregulation in glaucoma. Exp Eye Res 2015;133:112-25.
Rasoulinejad SA, Meftah N, Maniati MS, Maniati M. High levels of FBS and HbA1c and their association with diabetic retinopathy: a study in the north of Iran. J Diabetes Metab Disord 2022;21:399-406.
Wang S, Bao X. Hyperlipidemia, blood lipid level, and the risk of glaucoma: a meta-analysis. Invest Ophthalmol Vis Sci 2019;60:1028-43.
Atchison EA, Wood KM, Mattox CG, Barry CN, Lum F, MacCumber MW. The real-world effect of intravitreous anti–vascular endothelial growth factor drugs on intraocular pressure: an analysis using the IRIS Registry. Ophthalmology 2018;125:676-82.
Gabrielle PH, Nguyen V, Wolff B, et al. Intraocular pressure changes and vascular endothelial growth factor inhibitor use in various retinal diseases: long-term outcomes in routine clinical practice: data from the Fight Retinal Blindness! Registry. Ophthalmol Retina 2020;4:861-70.
Luo XY, Dai W, Chee ML, et al. Association of diabetes with central corneal thickness among a multiethnic Asian population. JAMA Netw Open 2019;2:e186647.
Kim YJ, Kim TG. The effects of type 2 diabetes mellitus on the corneal endothelium and central corneal thickness. Sci Rep 2021;11:8324.
Yassin SA, Al-Tamimi ER. Age, gender and refractive error association with intraocular pressure in healthy Saudi participants: a cross-sectional study. Saudi J Ophthalmol 2016;30:44-8.
Nannini D, Torres M, Chen YD, et al. African ancestry is associated with higher intraocular pressure in Latinos. Ophthalmology 2016;123:102-8.
Sperling S, Stokholm L, Thykjær AS, et al. Bidirectional 5‐year risks of diabetic retinopathy, glaucoma and/or ocular hypertension: results from a national screening programme. Acta Ophthalmol 2023;101:384-91.