Analyzing incoming page timestamps to estimate trainee sleep patterns
Main Article Content
Abstract
Purpose
Sleep deprivation is highly prevalent among surgical trainees and associated with decreased clinical performance. The goal of this study was to demonstrate a method of analyzing incoming page timestamps to estimate the sleep patterns of trainees during a home-call shift.
Methods
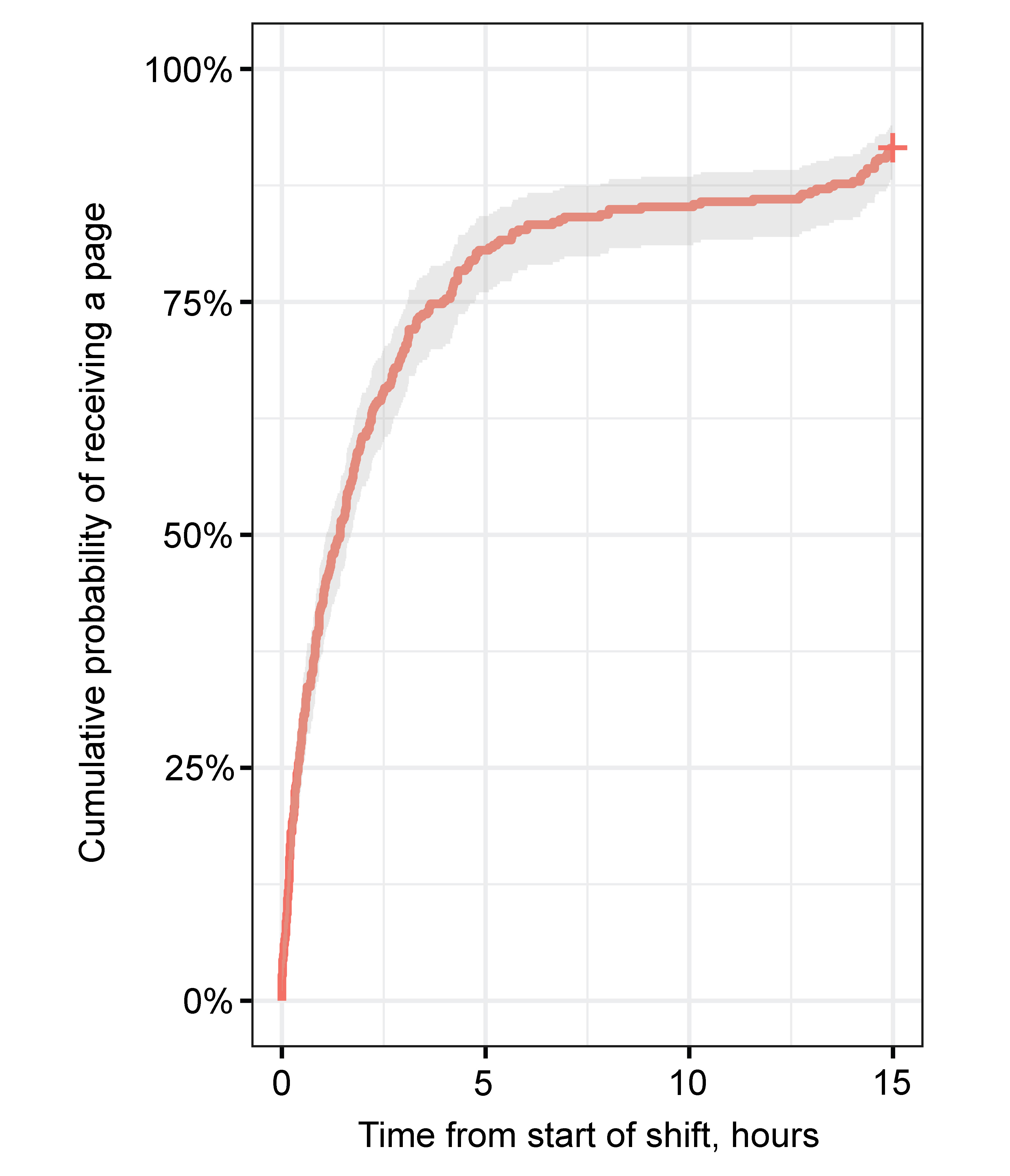
This was a retrospective study of all incoming pages to an Ophthalmology Service at a single tertiary care hospital from January 1, 2019, to December 31, 2019. The time and date of each incoming communication was recorded. The Kaplan-Meier estimator was used to determine the cumulative probability of receiving a page over the course of an at-home call shift.
Results
The mean number (± standard deviation) of incoming communications received during an overnight home-call shift (5 p.m.-8 a.m.) was 3.5 ± 2.5 (range, 0-15). The median time to first page was 1.4 hours (IQR, 0.4–4.0 hours). There was a significant difference between the number of pages received on weekdays compared to weekends (4.0 ± 2.5 vs 2.3 ± 2.1; P < 0.001). The cumulative probability of receiving a page during a shift was 91.5% (95% CI, 88.1%-95.6%). The probability of a 9-, 8-, 7-, or 6-hour interval without receiving an incoming page was 63.7%, 71.7%, 80.8%, and 87.6%, respectively.
Discussion
Analyzing timestamps may serve as a valuable tool for training programs to design home-call schedules that optimize the sleep patterns of trainees and ensure that fatigue does not negatively impact the quality of education and patient care.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Thomas, N. K. Resident burnout. JAMA 2004;292:2880-9.
Block L, Wu AW, Feldman L, Yeh HC, Desai SV. Residency schedule, burnout and patient care among first-year residents. Postgrad Med J 2013;89:495-500.
Kemper KJ, Schwartz A, Wilson PM, et al; Pediatric Resident Burnout-resilience Study Consortium. Burnout in pediatric residents: three years of national survey data. Pediatrics 2020;145:e20191030.
Chaukos D, Chad-Friedman E, et al. Risk and resilience factors associated with resident burnout. Acad Psychiatry 2017;41:189-94.
Philibert I. Sleep loss and performance in residents and nonphysicians: a meta-analytic examination. Sleep 2005;28:1392-402.
Nasca TJ, Day SH, Amis ES Jr; ACGME Duty Hour Task Force. The new recommendations on duty hours from the ACGME task force. N Engl J Med 2010;363:e3.
Antiel RM, Thompson SM, Reed DA, et al. ACGME duty-hour recommendations—a national survey of residency program directors. N Engl J Med 2010;363:e12.
Accreditation Council for Graduate Medical Education. Common Program Requirements (Residency). 2018. https://www.acgme.org/programs-and-institutions/programs/common-program-requirements/.
Caulley L, Quimby AE, Barrowman N, Moreau K, Vaccani J-P. Effect of home-call on otolaryngology resident education: a pilot study. J Surg Educ 2017;74:228-36.
Ronan JC. Decreasing resident physician burnout requires a multifaceted approach. Pediatrics 2020;145:e20193210.